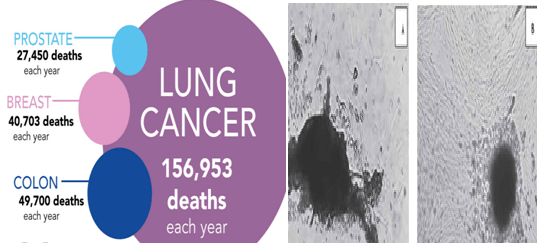
According to the World Health Organization, cancer was accountable for the deaths of 9.6 million deaths across the world in 2018! It goes on to say that 2.09 million cases of cancer are that of the lung which accounts for 1.76 million deaths. Apart from the loss of valuable human lives, the disease caused an expenditure of US$ 1.16 trillion in 2010! Research in CA: a Cancer Journal for Clinicians reported that 85% of lung cancer occur in individuals above 65 years of age and 60% of lives are lost.
The diagnosis of cancer currently involves many procedures ranging from examining the morphology to molecular analysis to cytogenetics to immunohistochemistry (IHC). Such multiple tests require significant amounts of sample tissues for testing. The diagnosis in the case of lung cancers is mainly bronchoscopy coupled with biopsies (endo/transbronchial). There are surgical approaches for diagnosing lung cancer like video-assisted thoracic surgery (VATS), thoracoscopy and mediastinoscopy. It is recommended by clinicians to initiate diagnosis using an approach that requires less tissue and minimum invasion.
In order to assist the understanding of lung cancer, given its grim grip on mankind, one system is the use of lung cancer cell primary culture along with the use of immortalized cell lines. Cell lines are often homogenous in terms of growth and functions and are easily available. 2010-published research by Gazdar and team in the Journal of the National Cancer Institute reported the success in cell lines representing lung cancers to facilitate studies. The use of the immortalized cells involves the process of “immortalization” that is associated with genetic alterations that in turn can influence the morphology and functioning of the cells. Hence, they may not be an accurate glimpse of in vivo conditions.
The biology (biochemistry and morphology) of primary lung cancer cell cultures are on the same lines of the tumours from which they are established. Thus, a team led by Angélica Herreño published a protocol to isolate Primary Cell Cultures from lung cancer samples obtained with minimum invasion called percutaneous needle biopsy. This becomes significant given that there are reports of establishing cultures from samples obtained using invasive approaches such as VATS. The approach of percutaneous biopsy is not only minimally invasive but also accurate and has been used to guide treatment.
Isolated tumour samples were washed and cut up in DMEM/F12 culture medium supplemented with 5% foetal bovine serum and 1% streptomycin/penicillin followed by culturing the fragments. The protocol resulted in 85% success in establishing cultures. Genetic analysis revealed genetic abnormalities as well as EGFR number aberrations representative of the heterogeneity of lung cancers. The phenotype could also be confirmed using the expression of markers such as NAPSIN, P63 and CK7.
Such molecular classification of tumours can assist decisions to treat lung cancer. A potential approach to treat non-small cell lung cancer (NSCLC) is such classification of the disease using mutations into groups that can then guide appropriate treatment. Research (Roberti et al, 2019) has pointed out the involvement of epigenetic alterations in tumour development. Thus, the identification of such molecular alterations using primary cultures can facilitate diagnosis and treatment.
References:
https://www.who.int/news-room/fact-sheets/detail/cancer
Siegel, R., Miller, K., Jemal A. (2006) Cancer statistics, 2006. CA: a Cancer Journal for Clinicians, 56(2), 106–130.
Gazdar, A. F., Girard, L., Lockwood, W. W., Lam, W. L., & Minna, J. D. (2010). Lung cancer cell lines as tools for biomedical discovery and research. Journal of the National Cancer Institute, 102, 1310–1321.
Angélica M. Herreño, María J. Fernández, Laura Rey, Juan A. Mejía, Alejandra Cañas, Olga M. Moreno, Berta Henríquez, Martín A. Montecino & Adriana P. Rojas | Ugo Rovigatti (Reviewing editor) (2018) Primary lung cancer cell culture from transthoracic needle biopsy samples, Cogent Medicine, 5:1.
Roberti, A., Valdes, A.F., Torrecillas, R. et al. Epigenetics in cancer therapy and nanomedicine. Clinical Epigenetics 11, 81 (2019).