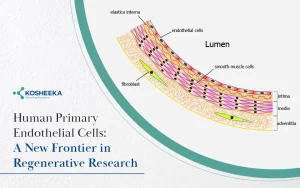
Endothelial cells are the thin inner lining of blood vessels. Endothelial cells regulate blood flow and maintain tissue homeostasis. Dysfunction of endothelial cells causes chronic diseases like ischaemic heart disease and stroke. These cells act as a selective barrier for immune cells, gasses, fluids, waste products, nutrients, and various molecules.
Endothelial cells play a crucial role in angiogenesis i.e. formation of new blood vessels from pre-existing vessels. Angiogenesis is essential for growth, development, and wound healing. During inflammation, endothelial cells help immune cells to selectively migrate toward the inflammation site. Endothelial cells also help in blood coagulation by regulating coagulation factors. Endothelial cells can be either primary cells isolated from biopsies or can be derived from Human induced pluripotent stem cells (iPSCs).
Primary Human Endothelial Cell
Primary human endothelial cells are isolated from the umbilical vein, coronary arteries, aorta, microvasculature, vascular tissues, etc, and retain most of the in vivo endothelial cells’ functional characteristics. These cells are widely used in angiogenesis, vascular diseases, wound healing, vascular permeability, and high throughput drug studies. The usage of these primary cells is limited by limited in vitro life span and donor variability. These challenges compel the use of alternative cell sources for long term studies and large-scale applications.

Human iPSCs-Derived Endothelial Cells
Human iPSC-derived endothelial cells are renewable cell resources, limiting donor variability. Human iPSCs can be generated from various somatic cells which are then differentiated into virtually all cell types including endothelial cells (Chitrangi et al, 2023) using specific culture conditions and growth factors. These cells can be generated from patients’ own cells, opening avenues for personalized therapy, and limiting the risk of immune rejection. These cells are widely used for vascular disease modeling, high-throughput drug screening, regenerative medicine, etc. Differentiation of iPSC towards functional endothelial cells needs a very robust optimized protocol. Additionally, these cells are prone to develop genetic and epigenetic abnormalities.

Characterization of Endothelial Cells
- Morphological Analysis: Endothelial cells are observed under a phase contrast microscope for general morphological analysis and confluence. Ultrastructural analysis at high resolution is performed by Electron Microscopy. Atomic Force Microscopy (AFM) measures cell stiffness and mechanical properties.
- Qualitative cell surface marker expression: Visualization of protein expression and localization by immunofluorescence or immunocytochemistry by detecting endothelial-specific markers like CD31 (PECAM-1), von Willebrand factor (vWF), and VE-cadherin (CD144).
- Quantitative cell surface marker expression: Quantitative analysis of cell surface markers by CD31, CD34, CD144, and CD146.
- Gene expression analysis: By RT-PCR (Reverse Transcription Polymerase Chain Reaction) or qPCR (Quantitative PCR) to quantify mRNA levels of endothelial-specific genes. RNA-sequencing provides the complete transcriptome analysis.
- Protein expression analysis: By western blot to quantitate and detect specific endothelial cell markers. By ELISA (Enzyme-Linked Immunosorbent Assay) to quantify specific secreted proteins e.g. Human ESM1.
- Functional Assays: By Tube Formation Assay or in vitro angiogenesis by assessing the ability of endothelial cells to form capillary-like structures in vitro. By wound healing (Scratch) assay by assessing cell migration to fill the scratch. By in vitro Permeability assay to evaluate the integrity of the endothelial cells’ monolayer.
Applications of Endothelial Cells
Endothelial cells play a pivotal role in various physiological and pathological functions, making them a valuable tool for multiple applications.
- Vascular Grafts: Cardiovascular disease is one of the most lethal diseases, which requires replacement or revascularization using vascular grafts. Autologous grafts are limited by quantity and quality. Innovative vascular tissue engineering methodologies such as three dimensional (3D) bioprinting or synthetic polymer scaffold are used for vascular grafts.
- Organ-on chip Models: Endothelial cells are incorporated into microfluidic devices to create organ-on-a-chip models that mimic the physiological environment of human organs more precisely. These models are useful in high throughput drug screening, disease modeling, etc, to study drug safety and efficacy. Endothelial cells are particularly used to study drugs for cardiovascular diseases.
- Wound healing: Endothelial cells promote wound healing by angiogenesis. Engineered constructs containing endothelial cells are used for chronic wound healing.
- Neurological diseases: Exosomes secreted from endothelial cells help in nervous system impairment. It’s reported that exosomes from human endothelial cells prevented neural injury (Yue et al, 2019).
- Vascular Biology Research: To study the mechanism of angiogenesis i.e. formation of new blood vessels from pre-existing vessels. To study the mechanism of vascular permeability, regulation of blood pressure, etc. Endothelial cells are widely used to study vascular disease mechanisms and develop novel therapies for vascular diseases.
- Disease Modelling: CRISPR-based gene editing and advanced bioprinting can further enhance the utility of endothelial cells in research and clinical applications. CRISPR-based gene editing tools enable the study and treatment of inherited vascular diseases such as Hereditary hemorrhagic telangiectasia. Endothelial cells are used to develop in vitro models for diseases like atherosclerosis, hypertension, and diabetic vasculopathy to understand disease mechanisms and their potential cures. These cells are also used to study tumor angiogenesis.
- Personalized or cell-based Therapies: Personalized therapies are developed by using patient-specific iPSC-derived endothelial cells. Endothelial cell-based therapies promote vascular regeneration in chronic wounds, ischemic heart diseases, etc.
- Regenerative Medicine: Endothelial progenitor cells have the potential for vascular regeneration.
- Immunology and Inflammation studies: Endothelial cells regulate the recruitment of immune cells in inflammation sites. These cells are an important research tool to investigate the role of endothelium in inflammation.
- Biomarker Discovery: Endothelial cells are used to discover various prognosis and diagnosis markers of cardiovascular diseases.
- Nanomedicine: Nanomedicine using endothelial cells is a promising tool in medical treatments and targeted drug delivery, due to its role in vascular biology.
At Kosheeka (a branch company of Advancells Group), we provide well-characterized, ready-to-use Human Endothelial Cells. These cells are amenable to high throughput drug screening, high-content imaging, disease modeling, tissue engineering, in vitro angiogenesis studies, wound healing (scratch) assay, gene expression profiling, etc. We can customize the pack size as per customer’s requirements.