Injuries in central and peripheral nervous system result in paralysis, anesthesia, disturbance of consciousness, and lack of motor control. Due to a limited ability of repair in case of neural damage, patients have to suffer from neurological diseases and their various after-effects. Human embryonic stem cells, induced pluripotent stem cells, and mesenchymal stem cells have all demonstrated regenerative effects on nervous system damage such as stroke, Parkinson’s, spinal cord injury etc. These stem cells can differentiate into functional neural cells, like neuron and glia cells. While embryonic stem cells and embryonic neuronal progenitors have ethical issues, and induced pluripotent stem cells are limited due to their carcinogenic potential, mesenchymal stem cells have been reported to be well suited as therapeutics.
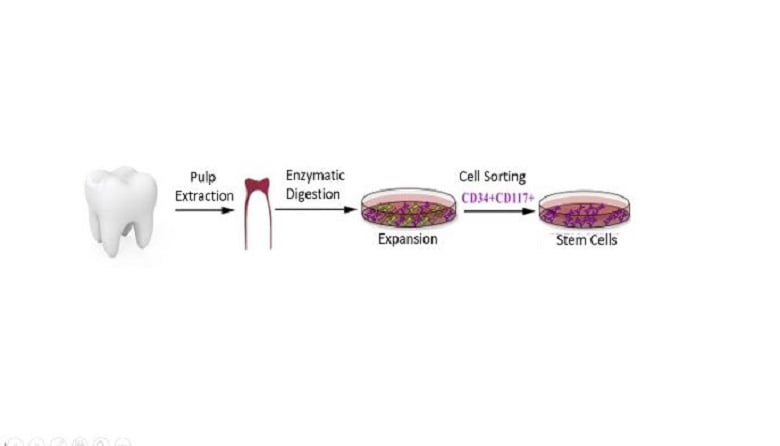
Human dental mesenchymal stem cells are commonly obtained from extracted third molars, primary teeth and the usually discarded surrounding tissues. Human dental mesenchymal stem cells have been reported to express embryonic markers and also exhibited multipotency such as myogenic, adipogenic, neurogenic, melanocytic, osteogenic, and odontogenic cells for regenerative dental therapies. When it comes to neural damage repair, the advantages of dental tissue-derived stem in neural regeneration are not only their ability to differentiate into neural cell lineage but also the simplicity of harvesting the stem cells. Additionally, human dental mesenchymal stem cells display better neural stem cell regeneration properties than bone marrow or adipose-derived mesenchymal stem cells.
Neural Crest and Dental Pulp Mesenchymal Stem Cells
The dental mesenchyme is the origin for most dental cells, and is known to be derived from neural crest cells. After interacting with the ectoderm (epithelium) inside the developing oral cavity, dental mesenchyme gives rise to dental pulp, dentin, periodontium, and the surrounding tissues. Especially 90% cells inside the dental pulp, originate from the neural crest cells. The nerve growth factor receptor (p75) is widely expressed in human dental pulp tissue. Additionally, human dental mesenchymal stem cells have been demonstrated to have self-renewing capacity besides differentiating into other neural crest-derived cells, therefore suggesting that dental pulp retains features of neural cells and therefore can be a much better therapeutic option for neural regeneration and repair.
Human Dental Mesenchymal Stem Cells and Neural Regeneration
Human dental pulp mesenchymal stem cells have been recorded to exhibit a voltage-gated, tetrodotoxin-sensitive inward current by the patch-clamp recording technique. These cells show glial cell marker GFAP, suggesting that dental pulp contains cells with similar properties of neuronal cells. Subsequent research reported that human dental pulp mesenchymal stem cells express neuronal markers nestin, bIII-tubulin, GFAP, and NF-200 at both the mRNA and protein levels. Under neural induction, these cells have been shown to differentiate into neuronal cells but without appropriate stimulation, human dental pulp mesenchymal stem cells can only differentiate to progenitor cells stage. Reports show that the activation of the cAMP and PKC signaling pathways can promote the differentiation of human dental pulp mesenchymal stem cells into functional neuron and glia cells.
Endogenous neural regeneration and repair is considered the best way for neural functional reconstruction and restoration and this repair is done by neural progenitor cells migrating to the injury site to go through plasticity changes, establish synaptic connection, and subsequently recover neural functionality. But in natural situation, inflammation during injury often hinders this process and alters the microenvironment to limit the transplanted progenitors till glial cell formation without establishing the neural network for functional recovery. Therefore, transplanting human dental pulp mesenchymal stem cells gives a therapeutic advantage of promoting neuronal cells to survival besides differentiating into neuronal progenitors and mature neurons. These dental pulp mesenchymal stem cells also provide immunomodulatory support to the damaged site to limit inflammation and in turn, promote survival of neurons to recover neuronal functionality.
If your lab is working on mesenchymal stem cells-based therapeutic research, visit https://kosheeka.com/product/human-dental-mesenchymal-stem-cells-hdmscs/ for procuring your flask of human dental pulp mesenchymal stem cells. For more information, mail us at info@kosheeka.com with your cell culture requirements.